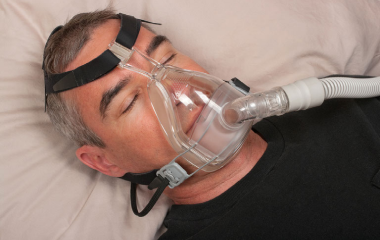
If you have obstructive sleep apnea, you may be wondering if your health care insurance will cover the cost of a CPAP machine. The short answer is – probably.
Most private health insurance policies cover positive airway pressure (PAP) equipment, like CPAP machines and masks. The level of coverage and the rules for coverage depend on your specific insurance policy.
Medicare typically covers a three-month trial for PAP therapy. If you use the treatment consistently, then you will qualify to keep using the machine.
Your insurance provider might make you buy or rent your PAP machine. If you have a high-deductible insurance plan and will be paying a lot right away for your machine, you might choose to pay it yourself without using your insurance. This is the “self-pay” option, which could be cheaper.
Most durable medical equipment (DME) providers and online stores have lower prices for cash purchases compared to those bought through insurers. If you choose to do self-pay, you don’t have to follow adherence regulations from your insurer.
Adherence
CPAP “adherence” – also called “compliance” – refers to how often you use your machine. Your adherence data is transmitted by your CPAP machine to the DME company or office where you got your device. This data is shared with your health insurance provider.
The insurer will monitor your adherence data. If you don’t use CPAP regularly, the insurer may stop paying for the CPAP machine. The insurer also may require that you return it and buy your own CPAP machine.
The Centers for Medicare and Medicaid Services (CMS) has specific adherence rules during the first three months of usage. CMS requires you to use your machine for at least 4 hours per night on 70 percent of nights during a consecutive 30-day period. This means that in a 30-day period, you must have used your machine for at least 4 hours on at least 21 days. Many private insurers also follow these CMS rules. You should check directly with your insurer to confirm its specific adherence requirements.
Talk to your medical provider if you’re having trouble with your CPAP machine. Notify your provider if you feel like the treatment is not helping you. Contact an AASM-accredited sleep center if you need more help. It’s important to ensure that your treatment is effective.